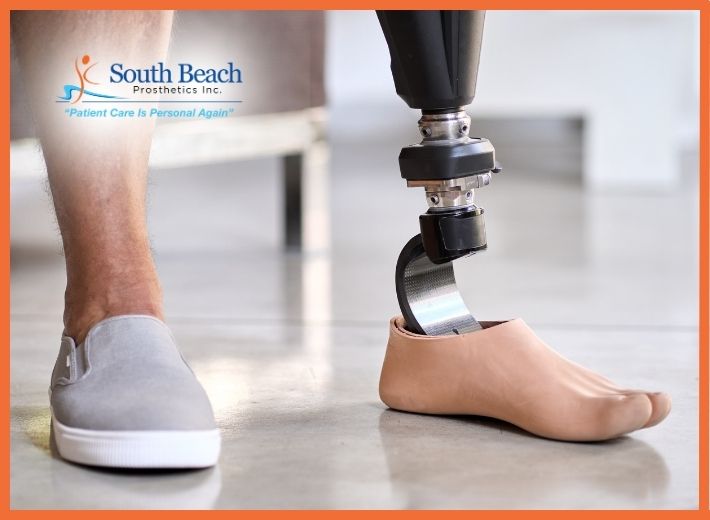
When you receive a prosthetic limb, one of the most important parts is also the part you might think about the least at first: the socket. The socket is the interface between your body and your prosthetic device. It is custom-shaped to your residual limb and designed to support your weight, provide stability, and allow comfortable movement. Yet almost every person who uses a prosthesis goes through a period of adjustments and tweaks. That is not a sign of failure. It is a sign of normal, healthy progress.
Understanding why adjustments are expected and how they help can remove a lot of uncertainty and frustration. It can help you know what to watch for, and when to reach out to your prosthetist. Most importantly, it can help you feel more confident in your recovery and mobility journey.
Why Sockets Change Over Time
One common misconception is that once a socket is made, it should remain the same forever. That is not how it works, and here is why.
Your residual limb is not a static shape. After amputation, the limb changes significantly, especially in the first year. Swelling goes down, tissues settle, muscle mass changes, and overall limb volume can shrink or expand slightly depending on activity and time of day. Some research finds that residual limb volume can change dramatically in the early stages of recovery, and continue fluctuating based on activity and health conditions.
Even in the long term, weight gain or loss, muscle use, and natural body rhythms can change how your limb fits inside a socket. Because a prosthetic socket is hard and rigid by design, it cannot automatically adapt to these changes. This is one of the main reasons adjustments are a normal part of ongoing care.
When you first start wearing a prosthetic limb, you may notice that the socket feels snug in the morning but looser later in the day. That is because your limb’s soft tissues respond to daily activity and fluid shifts. Over weeks and months, the goal is to allow the socket to evolve with your body so it continues to support you under different conditions.
What Happens During the Early Fitting Period
Right after receiving a new socket, you might experience areas of pressure, points that feel tight, or sections that feel loose. Some users even report skin irritation or redness after a day’s wear. These are not reasons to panic. They are signals from your body that help your prosthetist fine-tune the fit.
Pressure sores, skin irritation, or calluses often occur when certain areas of the limb experience too much friction or uneven pressure. Adjustments can redistribute that pressure and improve comfort.
Another common issue is socket movement or looseness. If your limb slides up and down inside the socket, or rotates as you walk, it means the suspension system or fitting is not supporting the limb as it should. That movement is not only uncomfortable, it can cause friction and lead to skin issues.
Some people also notice changes in how they balance or walk. If your gait feels off, you feel unstable on uneven ground, or your back or hips fatigue quickly, socket fit may be affecting your posture. A properly aligned socket improves not only comfort, but also overall posture and balance.
Why Adjustments Are Actually a Good Thing

This iterative process is part of creating a socket that:
- Feels secure when you put it on
- Distributes pressure evenly across the limb
- Supports balance and natural walking patterns
- Prevents skin damage and discomfort
Because limb volume changes are expected, many prosthetists start with a test socket or make several adjustments before finalizing. That does not mean something went wrong. It means the system is responsive and dynamic, not rigid and fixed. Over time, as the limb stabilizes, the number of needed adjustments usually decreases.
Many prosthetic users also rely on prosthetic socks or liners to help with daily volume fluctuations. These are not like everyday socks. They are specially made to add or remove padding that helps your socket adapt to a slightly larger or smaller residual limb. Over time, as your limb volume stabilizes, you may need fewer layers. But even that tells you something valuable about how your body is adjusting.
Adjustments Keep You Moving
Socket adjustments matter because they help you move more naturally and comfortably. A perfect socket fit improves your gait, confidence, and overall mobility. When the socket matches your limb’s shape and volume correctly, your body does not need to compensate with unnatural movements. That preserves your joints, muscles, and posture over the long term.
In contrast, a socket that is too tight can restrict circulation and numb the limb. A socket that is too loose can cause instability and excessive friction. Both conditions can lead to skin issues, discomfort, and avoidance of wear — and that can slow down your rehabilitation and daily life goals.
Adjustments are not about inconvenience. They are about precision, comfort, and long-term success.
How Your Prosthetist Monitors Fit and When to Ask for Help
After the initial socket is made, your prosthetist doesn’t stop paying attention to fit just because the device was delivered. In fact, much of the early care journey revolves around watching how your residual limb and socket interact over time. During follow-up appointments, your prosthetist will observe how your limb contacts the socket, how pressure is distributed, and how you walk and stand. They physically examine the internal shape of the socket and compare it with your limb to see whether there are uneven spots where pressure might build up or areas where the limb is pulling away from the socket. They also watch you move, because how your gait feels and how your balance shifts can reveal subtle alignment or fit issues that may not show up when you first sit down or stand still.
Everyday changes in your body can affect fit in ways that your prosthetist uses this information to address. Your residual limb naturally changes shape and volume throughout the day. Fluid shifts from circulation, heat, time spent on your feet, and activity levels can make your limbs swell slightly in the morning and shrink by the afternoon. Even small changes, like increased activity or sitting for long periods, can cause these fluctuations. This means a socket that felt snug and comfortable earlier may feel tighter later in the day or looser after resting. Factors such as weight gain or loss, muscle conditioning, or even changes in hydration can influence fit over weeks and months. Because the socket is rigid and the body is dynamic, the interface between them is in constant negotiation to find a new balance that supports your comfort and mobility.
View this post on Instagram
These everyday changes are why checking in regularly matters. Your prosthetist is not only looking for current problems but also anticipating how your socket will perform when you walk on uneven ground or stand for longer periods. If a socket is too tight because of swelling, circulation can be restricted, and numbness or tingling may occur. If the socket becomes loose because the limb’s volume has decreased, the limb can shift inside, causing instability and increased friction that leads to irritation. Both conditions can affect balance, gait, and how confident you feel walking in different environments.
Knowing when to reach out is key. If you notice persistent redness that stays after removing the socket, blisters, calluses, or open soreness, these are signs that pressure points are forming and adjustments are needed before the skin breaks down further. Feeling like the prosthesis slips or shifts during walking, experiencing pain that does not go away with short rest, or noticing uneven wear on your prosthetic components are all valid reasons to contact your prosthetist. Changes in your daily routine, such as increased activity or a change in weight, can also mean it’s time for a check-in. These are not inconveniences; they are important feedback that helps your care team adapt the socket to your body’s current needs.
By combining professional evaluation with your own daily observations, prosthetists can fine-tune or, if necessary, reshape or redesign a socket so that it continues to support you comfortably. Good care means listening to what the body is communicating through fit and comfort, and what the prosthetist learns through a hands-on assessment. That partnership is what keeps your prosthesis working well as you move through recovery and beyond.
Final Thoughts
View this post on Instagram
A prosthetic socket is not a one-time solution. It is part of a journey — a daily companion that needs attention and care. Regular adjustments are not only normal, they are essential to ensure that your prosthesis remains comfortable, functional, and supportive of your goals.
At South Beach Prosthetics, we encourage open communication and regular follow-ups. Socket adjustments are not setbacks. They are milestones in your path to freedom, confidence, and mobility.
Embrace them as part of the process. Your body is dynamic, and your care should be too.