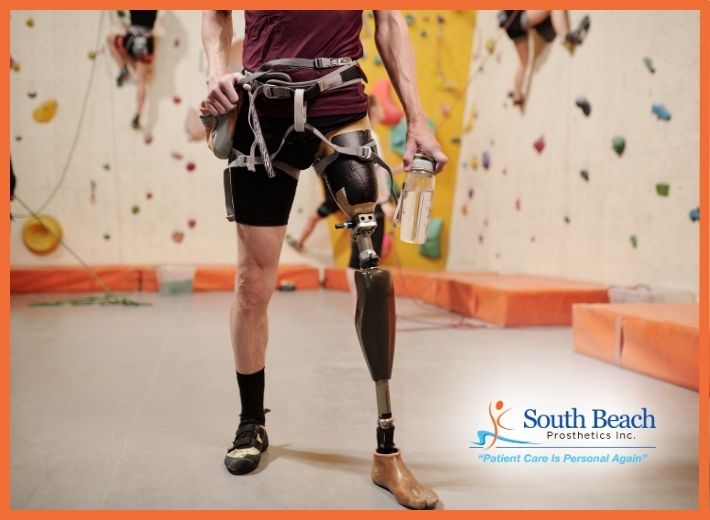
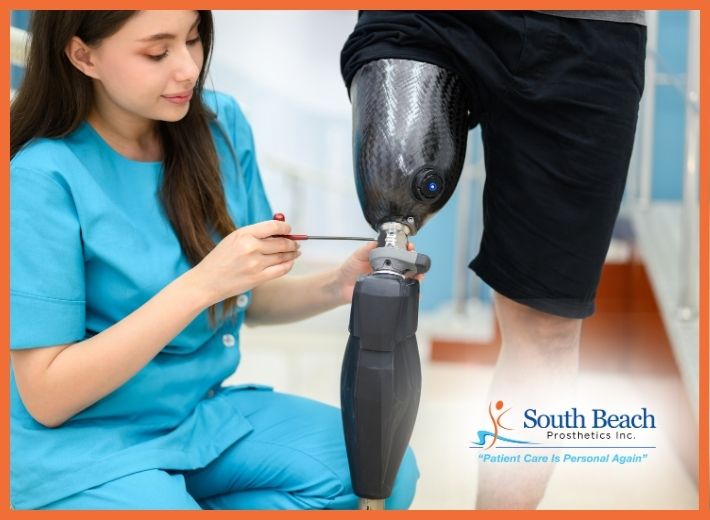
Getting a prosthetic limb is a big step in your life, and it helps to know what to expect along the way. At South Beach Prosthetics, we help you every step of the way, from your first evaluation to the day you take your first steps with your new prosthesis. Every patient is different, but knowing what to expect can help you feel less anxious and more focused on healing, making progress, and becoming independent.
Beginning with Your Evaluation
A full evaluation is the first step in your prosthetic journey. During your first visit, our team will ask you many questions about your health, lifestyle, daily activities, mobility goals, and medical history. This first talk is about more than just filling out forms. It helps us suggest prosthetic options that will best fit your lifestyle and goals.
We carefully look at your residual limb before even considering casting it. We look for swelling, sensitive spots, and bones that stick out because a well-fitting socket starts with a limb that is calm and stable. We’ll help you get the swelling down comfortably before we take any measurements if your limb is still swollen or changing.
Before the process of making a prosthetic can move forward, insurance companies may sometimes need to give their permission first. If that’s the case, your first visit might only be for evaluation and planning. We set up your casting appointment as soon as we get confirmation of your authorization and your limb is ready.
Casting and Measurements
The next step is casting, which you can do once your residual limb has reached a steady volume and your insurance has been checked. We make a physical cast of your residual limb and take exact measurements. These measurements are very important because they will be used to make your custom socket, which will be shaped to support weight and movement comfortably. We measure your non-amputated leg to ensure the prosthetic is the right height and balance.
For comfort, stability, and function, a well-made socket is essential. We can start making a diagnostic or test socket once we have the exact shape of your limb. This check socket lets us see how well the prosthesis fits and how well it lines up before it is finished.
Initial Fitting and Alignment
View this post on Instagram
The test socket comes to life on your second visit. This “check socket” is usually made of clear plastic that was made from your first cast. The clear material lets your doctor see how your limb fits inside and how the weight is spread out.
We also ask that you bring the shoes you plan to wear most often with your prosthesis to this appointment. This helps make sure that your alignment and walking patterns are correct. You will walk between two parallel bars while wearing the check socket so that our team can check your height, balance, comfort, and gait. We change the alignment if necessary to make you feel more stable and help you walk better.
Some patients need to go to more than one check socket and fitting visit. This is what we thought would happen. These steps let you make changes and fine-tune things so that your final prosthesis will fit and work well in everyday life.
Fitting and Delivery
Delivery day is the last step before you get your prosthesis. You and your practitioner will be sure that the test socket fits perfectly. You will get your custom prosthesis and a pair of prosthetic socks during this visit. These socks help you get the right fit as your limb changes size.
Your doctor will teach you how to put on your prosthesis and adjust for volume changes by adding or removing socks. Don’t expect to wear your first prosthesis all the time right away. We suggest starting with short periods of time wearing the item and then slowly increasing the time as you get used to it and feel more comfortable.
Early Use and Follow-Up Care
Once you begin using your prosthesis, follow-up care becomes a priority. During the early days of wear, check the skin on your residual limb often for redness or irritation. Redness that fades after removing the prosthesis over a broad area is typically normal, but a small spot of pressure that persists may indicate a need for adjustment. In that case, reach out to your practitioner as soon as possible.
We strongly recommend first-time prosthetic users engage in physical therapy. A physical therapist helps you learn how to walk, balance, and perform daily activities with confidence and stability. Therapy is an important part of lifelong success with your prosthesis.
Your practitioner will schedule a follow-up visit about one to two weeks after delivery to discuss how things are going and address any concerns. If you begin experiencing discomfort before that appointment, call our office to arrange an earlier visit.
It’s important to remember that if discomfort arises, it often relates to changes in the residual limb rather than an issue with the prosthesis itself. As your limb heals and changes, the fit inside the socket can shift. Adding or removing prosthetic socks often helps, but calling your practitioner ensures you make the right adjustments.
Coordinated Care and Support Services
At South Beach Prosthetics, we work with your doctors, physical therapists, home health providers, and even your family to make sure you feel supported every step of the way. We know that getting to appointments can be hard sometimes, so we offer free rides to all of your appointments, including hospital visits, doctor visits, rehab sessions, outpatient clinics, and prosthetic fittings. You don’t have to worry about logistics with this service; you can focus on getting better.
Our team also offers in-home care, so you can get help when you need it in the comfort of your own home.
 Your New Beginning
Your New Beginning
From the first evaluation to taking your first steps with a custom prosthesis, South Beach Prosthetics is committed to your success. We use state-of-the-art technology, including advanced casting and measurement tools, to ensure your prosthesis reflects your goals, lifestyle, and comfort needs. Our team of highly trained professionals is here to support you, educate you, and advocate for your best possible outcome.
Every step of the journey matters. Your prosthesis is not just a piece of technology, but a tool that helps restore confidence, mobility, and independence. We will work closely with you to address lower-limb pain, fitting challenges, and daily activity goals with a focus on personalized solutions.
If you are ready to begin your prosthetic journey or have questions about your next step, our team is here to help. Call us today at (888) 819-4721 to schedule your consultation and discover how South Beach Prosthetics can help you move forward with confidence.


 Your New Beginning
Your New Beginning
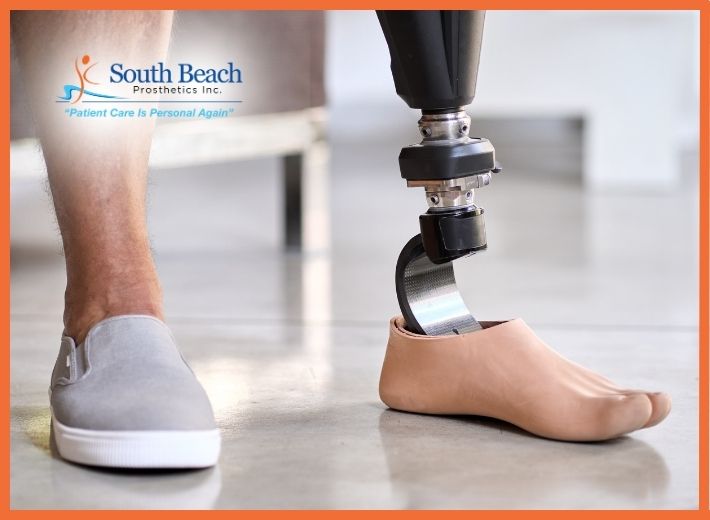


 1. Included transportation for all prosthetic and amputation-related appointments
1. Included transportation for all prosthetic and amputation-related appointments Transportation Included: So Nothing Holds You Back
Transportation Included: So Nothing Holds You Back Step Into 2026 with Confidence
Step Into 2026 with Confidence